Gordon Brown
The damage caused by COVID-19 – exacerbated by the continued appearance of new variants, most recently Omicron – has been catastrophic. More than five million lives worldwide have already been lost to COVID-19, and with confirmed cases on track to swell from 260 million today to 460 million by next autumn, the WHO estimates that five million more people may die from the disease in the coming months.
So, when the World Health Assembly (WHA) gathered for a special session that started November 29, its task was nothing less than preventing the recurrence of such a tragedy. Specifically, the world now needs an internationally binding agreement to prevent future infectious-disease outbreaks from becoming pandemics.
As Tedros Ghebreyesus, the WHO’s director-general, has argued, a new agreement should be underpinned by a high-level commitment to health for all, grounded in equity and solidarity between countries. Everyone, regardless of their wealth or income, should have fair access to what they need to maintain their health, and the international community should ensure the equitable use and distribution of available medical resources. That will require a fully functioning global surveillance system, fast-tracking and sharing support in emergencies, and predictable finance.
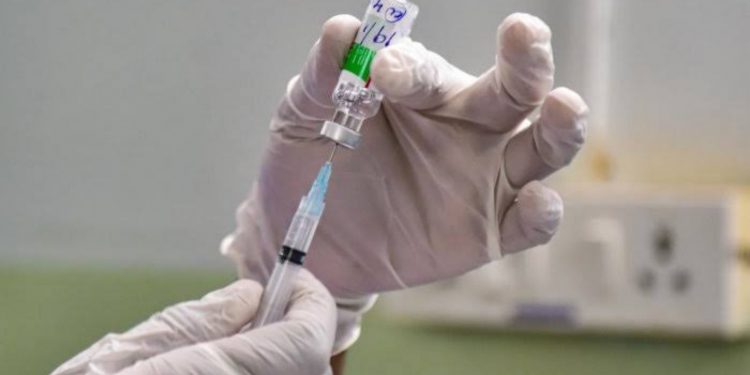
Nothing illustrates more clearly the need for such an arrangement than the world’s collective failure to ensure the promised equitable distribution of COVID-19 vaccines. Although brilliant science and a strong manufacturing effort mean that we will have produced 12 billion doses by the end of 2021 – enough to vaccinate every adult in the world – 95% of adults in low-income countries remain unprotected. This is perhaps the greatest public policy failure of our times.
The WHO’s internationally agreed target of vaccinating 40% of the adult population of every country by December 2021 looks set to be missed by 82 countries. On current trends, it will take until next Easter to get close to 40%, and even then, dozens of countries may fall short. In fact, since the G7 summit in June, when leaders pledged that the whole world would be vaccinated against COVID-19 by 2022, the gap between the vaccine haves and have-nots has widened rather than diminished.
In high-income countries, vaccination rates have risen from 40% in June to roughly 74% now, but they have increased at a glacial pace in low-income countries – from 1% to less than 5%. For every adult now being inoculated in a low-income country, six adults in middle- and high-income countries are receiving their booster shots. And 73% of African health workers remain unprotected.
True, important regional initiatives have taken steps to address the inequity gap. The African Union’s vaccine-purchasing facility, the African Vaccine Acquisition Trust, has bought 400 million single-shot vaccine doses from Johnson & Johnson and, thanks to the Trust’s chair, Strive Masiyiwa, and the US government, a further 110 million doses from Moderna, with 50 million to be delivered by March. But this is still not enough to meet the needs of Africa’s 1.3 billion people.
This inequality is not difficult to explain: a recent survey by Airfinity has shown that the world’s richest countries have bought 89% of all COVID-19 vaccines, and currently retain control of 71% of future deliveries. The Global North has fallen short of its pledges to donate vaccines to the Global South. The US has sent only 25% of what it promised, while the EU, the UK, and Canada have performed even worse, dispatching just 19%, 11%, and 5%, respectively, of their pledged doses. The COVID-19 Vaccine Global Access (COVAX) facility, which had hoped to distribute two billion vaccines by December, now expects to deliver just three-quarters of that amount.
Such is the scale of vaccine hoarding in rich countries that Airfinity estimates that by the end of 2021, 100 million doses in the G20 stockpile will pass their expiration date and be wasted. For G20 countries to hoard life-saving vaccines and deny them to the poorest countries, while allowing tens of millions of doses to go to waste, is a morally indefensible act of medical and social vandalism that should never be forgotten or forgiven.
Vaccine inequities show why more fundamental changes are needed in the international global public-health architecture of health decision-making. Of course, among international organisations, only the Appellate Body of the WTO and the International Criminal Court, whose decisions are final, have the freedom and authority to make binding decisions that national governments are obliged to follow. And because of that, these bodies are under assault from a coalition of anti-internationalists. Securing a binding treaty will not be easy.
There is already a global-health treaty to reduce tobacco demand and supply, and a 2011 agreement to ensure that the WHO can commandeer supplies of flu vaccine when needed. But the legally binding international pact necessary to enable global-health authorities to do more to prevent, detect, prepare for, and control a pandemic has so far eluded us. At a time when new variants of COVID-19 are appearing, it is imperative that the special summit launches a process to develop a legally binding agreement under the auspices of the WHO constitution.
A robust agreement should contain several key elements. First, global-health leaders must have more authority to develop and upgrade health surveillance. Second, we need to build on the pioneering work of the Access to COVID-19 Tools Accelerator (ACT-A) and COVAX, and ensure equitable manufacturing and distribution of personal protective equipment, tests, treatments, and vaccines, so that all countries can protect themselves better against current and future pandemics. Third, we need a global pandemic preparedness board.
But such arrangements will work only if leaders devise a sustainable financing mechanism to address the glaring global inequalities in health provision. Too often in times of global crises, we are reduced to passing the hat or convening ad hoc donor conferences. Ideally, pandemic preparedness should be financed according to a burden-sharing formula that allocates the costs among countries with the greatest capacity to pay. Even now, less than 20% of the WHO’s budget is covered in this way. The eradication of smallpox in the 1960s and 1970s was historic not least because the final push was initiated by a cost-sharing agreement among the richest countries.
Failure to meet global COVID-19 vaccination targets could cost $2.3 trillion in lost GDP by 2025. Given that prospect, the G20 high-level independent panel’s proposed $10 billion annual budget for pandemic prevention and preparedness would offer one of the greatest returns on investment in history. But we must act now – and this week’s WHA summit is the place to start.
The writer is a former Prime Minister of the United Kingdom. @Project Syndicate.