Peter Singer
Novak Djokovic, the world’s top-ranking tennis player, has just been granted a medical exemption to take part in the Australian Open. Djokovic, who has won the event nine times (one more victory would give him a record-breaking 21 major titles), refused to show proof of vaccination, which is required to enter Australia. “I will not reveal my status whether I have been vaccinated or not,” he told Blic, a Serbian daily, calling it “a private matter and an inappropriate inquiry.”
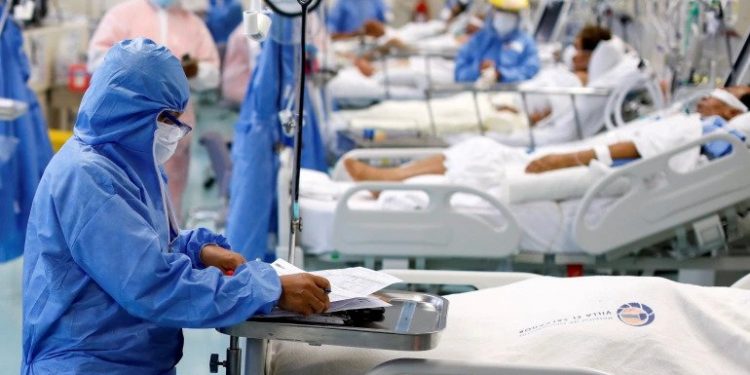
The family of Dale Weeks, who died last month at the age of 78, would disagree. Weeks was a patient at a small hospital in rural Iowa, being treated for sepsis. The hospital sought to transfer him to a larger hospital where he could have surgery, but a surge in COVID-19 patients, almost all of them unvaccinated, meant that there were no spare beds. It took 15 days for Weeks to obtain a transfer, and by then, it was too late.
Weeks became another of the many indirect victims of COVID-19 – people who never had the virus, but died because others who did were taking up scarce health-care resources, especially beds in intensive care units. His daughter said: “The thing that bothers me the most is people’s selfish decision not to get vaccinated and the failure to see how this affects a greater group of people. That’s the part that’s really difficult to swallow.”
Last month, Rob Davidson, an emergency room physician at a hospital in Michigan, wrote an essay for the New York Times that provided a vivid picture of life in a hospital that had consistently been at or near capacity for several weeks. The overwhelming majority of the patients had COVID-19, and 98% of those needing acute critical care were unvaccinated.
What happened to Weeks was happening at Davidson’s hospital, too: those in need of more specialised treatment could not be transferred to a larger facility because nearly every hospital in the region was already full or close to it. Davidson is unable to view the choice not to get vaccinated as a private matter. “It forces patients with ruptured appendixes and broken bones to wait for hours in my emergency department; it postpones surgeries for countless other people and burns out doctors and nurses.”
There has been considerable opposition to vaccine mandates – opposition that I have argued is misguided. With earlier variants, the unvaccinated are more likely to infect others. With the more contagious Omicron variant, the extent to which current vaccines reduce infection and the ability to spread the virus is less clear. But we do know that vaccination reduces the severity of the illness, and therefore the need for hospitalisation.
For the situation that Davidson described, and that Weeks’ children believe led to their father’s death, a different solution is available, one that respects the decisions of those who choose not to be vaccinated but requires them to bear the consequences of their choice. Hospitals that are at or near capacity should warn the populations they serve that, after a certain date – far enough in the future to allow ample time for people to get fully vaccinated – they will give vaccinated patients priority over unvaccinated patients with COVID-19.
After the announced date, when both a vaccinated and an unvaccinated patient with COVID-19 need the last available bed in the intensive care unit, the vaccinated patient should get it. If the last ICU bed is given to an unvaccinated patient because at the time there was no one else who needed it, and a vaccinated patient with a greater or equal need for the facility then arrives, the bed should be reallocated to the vaccinated patient.
The unvaccinated patient, or the family of that patient, may object. But if the move is in accord with a previously announced policy, and everyone had the opportunity to be vaccinated before the policy took effect, people who make choices that are likely to harm others, and have been warned of the consequences of those choices, must take responsibility for them.
Hospitals with sufficient capacity should, of course, continue to treat unvaccinated patients with COVID-19 as best they can. Despite the extra strain this puts on hospital staff, everyone should have sufficient compassion to try to save lives, even when those whose lives need saving have made foolish, selfish choices.
Exceptions should be made for those few patients for whom vaccination is contra-indicated on medical grounds, but not for those who claim to have religious grounds for exemption. No major religion rejects vaccination, and if some people choose to interpret their religious beliefs as requiring them to avoid vaccination, then they, and not others, should bear the consequences.
Such a policy is likely to increase vaccination rates, which will benefit the currently unvaccinated as well as the vaccinated, and save lives, just as vaccine mandates have saved lives by increasing the number of vaccinated people. But even if the policy does not persuade more people to get vaccinated, at least fewer people would die from health conditions over which they have no control because others who regard vaccination as a ‘personal choice,’ and selfishly rejected it, are using scarce resources needed to save lives.
The writer is Professor of Bioethics at Princeton University and Founder of the nonprofit organisation The Life You Can Save. ©Project Syndicate.